Female Internal Genital Organs
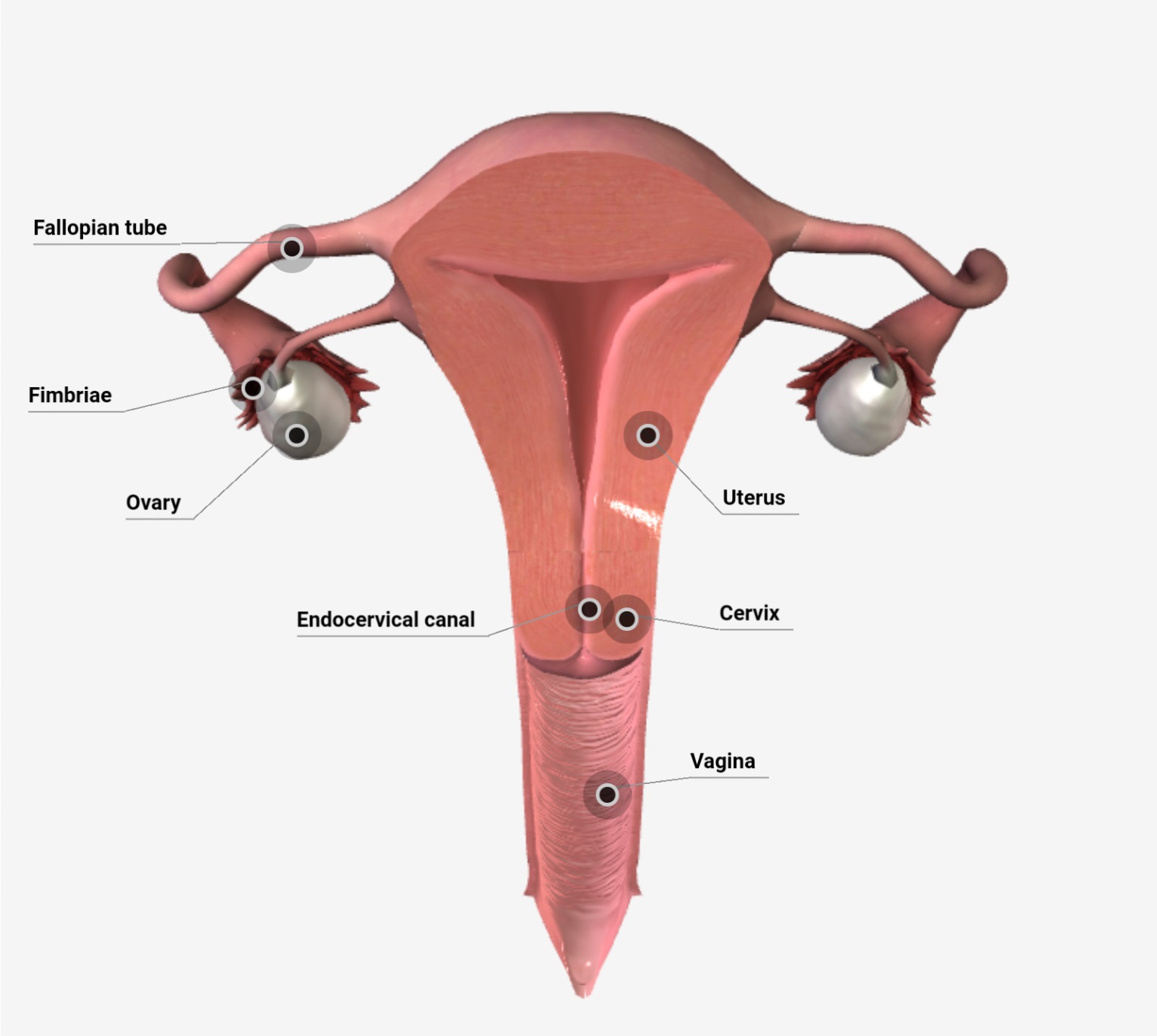
Female internal genitalia includes all the female reproductive organs which lie internally, are as follows-
A) Uterus
The uterus (womb) is the site of implantation of a fertilized ovum, Growth and development of the fetus during pregnancy and labor. During reproductive cycles when implantation does not occur, the uterus is the source of menstrual flow.
Anatomy-
- It is situated between the urinary bladder and the rectum, the uterus is the size and shape of an inverted pear. In a nonpregnant state, it is about 7.5 long, 5cm wide, and 2.5cm thick. Its position is anteverted (lean forward at a right angle to the vagina) and anteflexed (body of the uterus projects anteriorly and superiorly over the urinary bladder).
- Anatomical subdivisions of the uterus are – a dome-shaped portion superior to the uterine tubes called the fundus, a central portion called the body, an inferior narrow portion called the cervix that opens into the vagina. Between the body of the uterus and the cervix is the isthmus, a constricted region about 1 cm long. The interior of the body of the uterus is called the uterine cavity, and the interior of the cervix is called the cervical canal. The cervical canal opens into the uterine cavity at the internal os and into the vagina at the external os.
- Several ligaments that are extensions of the parietal peritoneum maintain the position of the uterus. These are-paired broad ligaments which are double folds of peritoneum attaching the uterus to either side of the pelvic cavity. The paired uterosacral ligaments, lie on either side of the rectum and connect the uterus to the sacrum. The cardinal (transverse cervical) ligaments extend from the pelvic wall to the cervix and vagina. The round ligaments are bands of fibrous connective tissue between the layers of the broad ligament.
- The uterus consists of three layers of tissue: perimetrium, myometrium, and endometrium. The outer layer—the perimetrium or serosa is part of the visceral peritoneum, laterally, it becomes the broad ligament. Anteriorly, it covers the urinary bladder and forms a shallow pouch, the vesicouterine. Posteriorly, it covers the rectum and forms a deep pouch between the uterus and rectum, the rectouterine pouch or pouch of Douglas. The middle layer of the uterus, the myometrium, consists of three layers of smooth muscle fibers that are thickest in the fundus and thinnest in the cervix. The middle layer is oblique, the inner and outer layers are circular and longitudinal. The inner layer of the uterus, the endometrium is highly vascularized and is divided into two layers. The stratum functionalis (functional layer) lines the uterine cavity and sloughs off during menstruation. The deeper layer, the stratum basalis (basal layer), is permanent and gives rise to a new stratum functionalis after each menstruation.
Blood supply-
- Branches of the internal iliac artery called uterine arteries to supply blood to the uterus. Uterine arteries give off branches called arcuate arteries. These arteries branch into radial arteries that penetrate deeply into the myometrium. Just before the branches enter the endometrium, they divide into two kinds of arterioles: Straight arterioles supply the stratum basalis spiral arterioles supply the stratum functionalis.
- Blood leaving the uterus is drained by the uterine veins into the internal iliac veins. The rich blood supply of the uterus is essential to support the regrowth of a new stratum functionalis after menstruation, implantation of a fertilized ovum, and development of the placenta.
B) Vagina
The vagina is a tubular, 10-cm long fibromuscular canal lined with a mucous membrane that extends from the body to the cervix. It is the receptacle for the penis during sexual intercourse, the outlet for menstrual flow, and the passageway for childbirth.
- It is situated between the urinary bladder and the rectum, the vagina is directed superiorly and posteriorly, where it attaches to the uterus. The mucosa of the vagina is continuous with that of the uterus and contains large stores of glycogen, the decomposition of which produces acids. The resulting acidic environment reduces microbial growth.
- A thin fold mucous membrane, called the hymen, forms a border around and partially closes the inferior end of the vaginal opening to the exterior.
C) Uterine tube-
Females have two uterine tubes, also called fallopian tubes or oviducts that extend laterally from the uterus. The tubes, measure about 10 cm long, lie within the folds of the broad ligaments of the uterus. They provide a route for sperm to reach an ovum and transport secondary oocytes and fertilized ova from the ovaries to the uterus.
- The funnel-shaped portion of each tube, called the infundibulum, is close to the ovary but is open to the pelvic cavity. It ends in a finger-like projection called fimbriae, one of which is longer than the other called ovarian fimbriae attached to the lateral end of the ovary.
- The ampulla of the uterine tube is the widest, longest portion, two-thirds of its length.
- The isthmus of the uterine tube is the more medial, short, narrow.
- The uterine tubes are composed of three layers-mucosa, muscularis, and serosa. The epithelium contains ciliated simple columnar cells, which function as a ciliary movement for a fertilized ovum (or secondary oocyte) within the uterine tube toward the uterus, Peristaltic contractions of the muscularis and the ciliary action of the mucosa help to move the oocyte or fertilized ovum toward the uterus.
- After ovulation, local currents are produced by movements of the fimbriae, which surround the surface of the mature follicle just before ovulation occurs. These currents sweep the ovulated secondary oocyte from the peritoneal cavity into the uterine tube.
- A sperm cell usually encounters and fertilizes a secondary oocyte in the ampulla of the uterine tube, Fertilization can occur up to about 24 hours after ovulation. Some hours after fertilization, the nuclear materials of the haploid ovum and sperm unite. The diploid fertilized ovum is now called a zygote and begins to undergo cell divisions while moving toward the uterus. It arrives in the uterus 6 to 7 days after ovulation. Unfertilized secondary oocytes disintegrate.
D) Ovaries
The ovaries are the female gonads, are paired glands that are similar to unshelled almonds in size and shape. The ovaries produce gametes, secondary oocytes that develop into mature ova after fertilization and release hormones, including progesterone and estrogens, inhibin, and relaxin.
- The broad ligament of the uterus, which is a fold of the parietal peritoneum, attaches to the ovaries by a double-layered fold of peritoneum called the mesovarium. The ovarian ligament attaches the ovaries to the uterus and the suspensory ligament attaches them to the pelvic wall. Each ovary contains a hilum, the point of entrance and exit for blood vessels and nerves.
- Each ovary consists of the following parts-
- The germinal epithelium is a layer of simple epithelium that covers the surface of the ovary.
- The tunica albuginea is a whitish capsule of dense irregular connective tissue located deep to the germinal epithelium.
- The ovarian cortex is a region just deep to the tunica albuginea which consists of ovarian follicles.
- The ovarian medulla is deep to the ovarian cortex but the medulla consists of connective tissue and contains blood vessels and nerves. Ovarian follicles are in the cortex and consist of oocytes in various stages of development or the cells surrounding them.
- When the surrounding cells form a single layer, they are called follicular cells, later in development, when they form several layers, they are referred to as granulosa cells. The surrounding cells nourish the developing oocyte and begin to secrete estrogens as the follicle grows larger.
- A mature follicle is a large, fluid-filled follicle that is ready to rupture and expel its secondary oocyte, this process is known as ovulation.
- A corpus luteum contains the remnants of a mature follicle after ovulation. The corpus luteum produces progesterone, estrogens, relaxin, and inhibin until it degenerates into fibrous scar tissue called the corpus albicans.
Download the App: Android App
For more Lectures, please visit-
YouTube Channel – NursingLecture
Facebook – Facebook Page
Check out the video of the Female Internal Genital Organs here: