Pituitary Gland
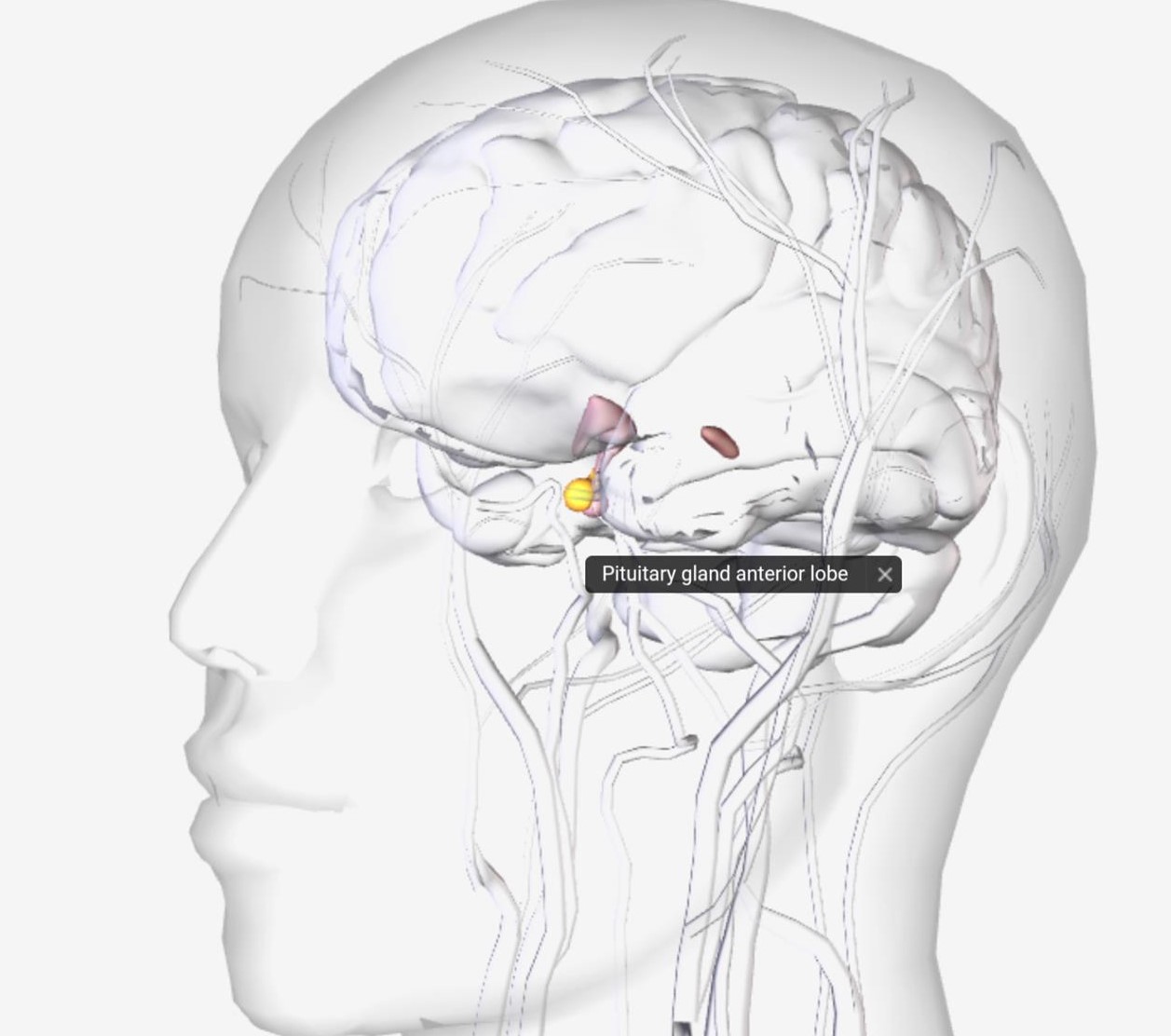
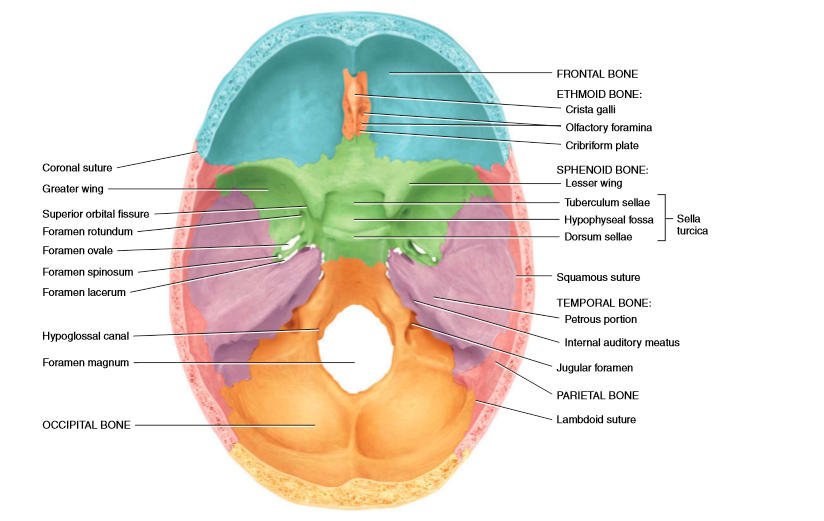
The pituitary gland is a pea-shaped structure that measures 1–1.5 cm in diameter and weight 0.5 gm lies in the hypophyseal fossa of the sella turcica of the sphenoid bone.
It attaches to the hypothalamus by a stalk, called infundibulum, and has two separate portions: the anterior pituitary and the posterior pituitary.
The anterior pituitary, also called the adenohypophysis, about 75% of the total weight of the gland, is composed of epithelial tissue. The posterior pituitary also called the neurohypophysis, is composed of neural tissue.
Anterior Pituitary
The anterior pituitary secretes hormones that regulate activities, from growth to reproduction. Anterior pituitary hormones are stimulated by releasing hormones and suppressed by inhibiting hormones from the hypothalamus.
Five types of anterior pituitary cells—Somatotrophs, Thyrotrophs, Gonadotrophs, Lactotrophs, and Corticotrophs.
1. Somatotrophs- Secrete human growth hormone (hGH), also known as somatotropin. Human growth hormone stimulates several tissues to secrete insulin-like growth factors(IGFs), which stimulates general body growth and regulates metabolism.
2. Thyrotrophs- Secrete thyroid-stimulating hormone (TSH), also known as thyrotropin. TSH controls the secretions of the thyroid gland.
3. Gonadotrophs- Secrete two gonadotropins- follicle-stimulating hormone (FSH) and luteinizing hormone (LH). FSH and LH both act on the gonads. They stimulate secretion of estrogens and progesterone and the maturation of oocytes in the ovaries and stimulate sperm production and secretion of testosterone in the testes.
4. Lactotrophs- Secrete prolactin (PRL), which initiates milk production in the mammary glands.
5. Corticotrophs- Secrete adrenocorticotropic hormone (ACTH), also known as corticotropin which stimulates the adrenal cortex to secrete glucocorticoids. also secretes the Melanocyte-stimulating hormone (MSH).
NOTE– Neurosecretory cells in the hypothalamus secrete five releasing hormones, which stimulate secretion of anterior pituitary hormones, and two inhibiting hormones, which suppress the secretion of the anterior pituitary hormone. Negative feedback of hormones released by target glands (when blood levels of their hormones rise) decreases secretions of anterior pituitary cell thyrotrophs, gonadotrophs, and corticotrophs.
1. Human Growth Hormone-
Somatotrophs releases human growth hormone (hGH). The function of hGH is to promote synthesis and secretion of small protein hormones called insulin-like growth factors. In response to human growth hormone, in the liver, skeletal muscles, cartilage, bones, and other tissues secrete IGFs, which may either enter the bloodstream from the liver or act locally in other tissues.
- IGFs cause cells to grow and multiply by uptake of amino acids into cells for protein synthesis. Which increases the growth rate of the skeleton and skeletal muscles during childhood and teenage years. In adults, it maintains the mass of muscles and bones and promotes healing of injuries.
- IGFs cause lipolysis (break down of lipid) in adipose tissue, which results in the use of the released fatty acids for ATP production.
- It influences carbohydrate metabolism by decreasing glucose uptake, so it is available to neurons for ATP production in times of glucose scarcity.
- IGF also stimulates liver cells to release glucose into the blood.
Control of secretion– Their Secretion is controlled mainly by growth hormone-releasing hormone (GHRH) promotes the secretion of human growth hormone, and growth hormone inhibiting hormone (GHIH) suppresses it.
2. Thyroid Stimulating Hormone-
Thyroid-stimulating hormone (TSH) stimulates the synthesis and secretion of the two thyroid hormones, triiodothyronine (T3) and thyroxine (T4), both produced by the thyroid gland.
Control of secretion-Thyrotropin-releasing hormone (TRH) from the hypothalamus controls TSH secretion but there is no inhibiting hormone, it depends on blood levels of T3 and T4.
3. Follicle Stimulating Hormone-
The ovaries are the targets for follicle stimulating hormone(FSH). FSH initiates the development of several ovarian follicles, that surround a developing oocyte and stimulates follicular cells to secrete estrogens in the female. FSH stimulates sperm production in the testes in the male.
Control of secretion- Gonadotropin-releasing hormone (GnRH) from the hypothalamus stimulates FSH release. The release of GnRH and FSH is suppressed by estrogens in females and by testosterone in males, through negative feedback systems but no gonadotroph inhibiting hormone.
4. Luteinizing Hormone
In females, luteinizing hormone (LH) triggers ovulation, the release of a secondary oocyte by an ovary. It stimulates the formation of the corpus luteum and the secretion of progesterone. Together, FSH and LH also stimulate secretion of estrogens by ovarian cells. Estrogens and progesterone prepare the uterus for the implantation of a fertilized ovum and help prepare the mammary glands for milk secretion. In males, LH stimulates Leydig cells to secrete testosterone.
Control of secretion- The secretion of LH, is controlled by gonadotropin-releasing hormone (GnRH).
5. Prolactin
Prolactin (PRL), together with oxytocin(released from the posterior pituitary), initiates and maintains milk production and ejection by the mammary glands.
Control of secretion The hypothalamus secretes both inhibitory and excitatory hormones that regulate prolactin secretion. Prolactin inhibiting hormone (PIH), which is dopamine, inhibits the release of prolactin from the anterior pituitary. During pregnancy, the prolactin level rises, stimulated by prolactin releasing hormone (PRH) from the hypothalamus. The sucking action of an infant causes a release of PRH.
6. Adrenocorticotropic Hormone-
Corticotrophs secrete adrenocorticotropic hormone (ACTH) which controls the production and secretion of cortisol and other glucocorticoids by the cortex of the adrenal glands.
Control of secretion- Corticotropin-releasing hormone (CRH) from the hypothalamus stimulates the secretion of ACTH by corticotrophs. Stress-related stimuli, such as low blood glucose or physical also stimulate the release of ACTH. Glucocorticoids inhibit CRH and ACTH release via negative feedback.
7. Melanocyte-Stimulating Hormone-
Melanocyte-stimulating hormone(MSH) increases skin pigmentation by stimulating the melanin granules in melanocytes. MSH for several days does produce a darkening of the skin.
Control of secretion Excessive levels of corticotropin-releasing hormone (CRH) can stimulate MSH release; dopamine inhibits MSH release.
Posterior Pituitary
-Posterior pituitary does not synthesize hormones, it does store and release two hormones. It consists of axon terminals of hypothalamic neurosecretory cells.
-The neuronal cell bodies synthesize the hormones oxytocin and antidiuretic hormone (ADH), also called vasopressin.
– After their production in the cell bodies of neurosecretory cells, the hormone is packaged into secretory vesicles, which move to the axon terminals in the posterior pituitary, where they are stored until nerve impulses trigger exocytosis and release of the hormone.
-Blood is supplied to the posterior pituitary by the inferior hypophyseal arteries, branch from the internal carotid arteries. drain into the capillary plexus of the infundibular process, From this plexus, hormones pass into the posterior hypophyseal veins for distribution to target cells in other tissues.
Two hormones are-
1. Oxytocin-
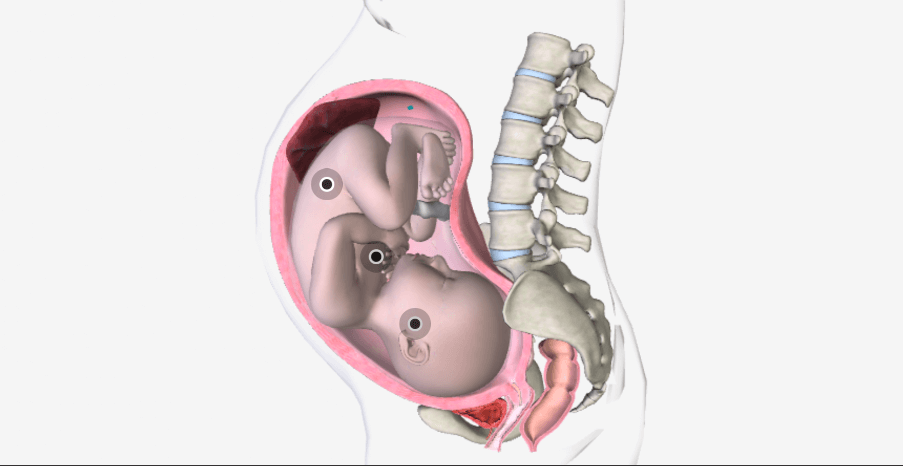
oxytocin affects two target tissues during and after delivery of a baby is the mother’s uterus and breasts. During delivery, stretching of the cervix of the uterus stimulates the release of oxytocin which causes contraction of smooth muscle cells in the uterus and after delivery, it stimulates milk ejection from the mammary glands in response to suckling effect.
2. Antidiuretic Hormone-
Antidiuretic causes the kidneys to return more water to the blood, thus decreasing urine output. ADH also decreases the water lost through sweating and causes constriction of arterioles, which increases blood pressure. another name, vasopressin, causes vessel constriction. The amount of ADH secreted varies with blood osmotic pressure and blood volume.
- High blood osmotic pressure (or decreased blood volume) due to dehydration stimulates osmoreceptors, in the hypothalamus that monitor blood osmotic pressure. Elevated blood osmotic pressure activates the osmoreceptors. which activate the hypothalamic neurosecretory cells that synthesize and release ADH. the neurosecretory cell generates nerve impulses that cause exocytosis of ADH-containing vesicles in the posterior pituitary. Then ADH diffuses into blood capillaries of the posterior pituitary and carries ADH to target tissues: the kidneys, sweat glands, and smooth muscle in blood vessel walls. The kidneys respond by retaining more water, which decreases urine output. sweat glands lower the rate of water loss by perspiration from the skin. Smooth muscle in the walls of arterioles contracts, which constricts the lumen of the vessel and increases blood pressure.
- The low osmotic pressure of blood (or increased blood volume) inhibits the osmoreceptors. Inhibition of osmoreceptors reduces or stops ADH secretion. The kidneys then retain less water by forming a larger volume of urine, the secretory activity of sweat glands increases, and arterioles dilate.