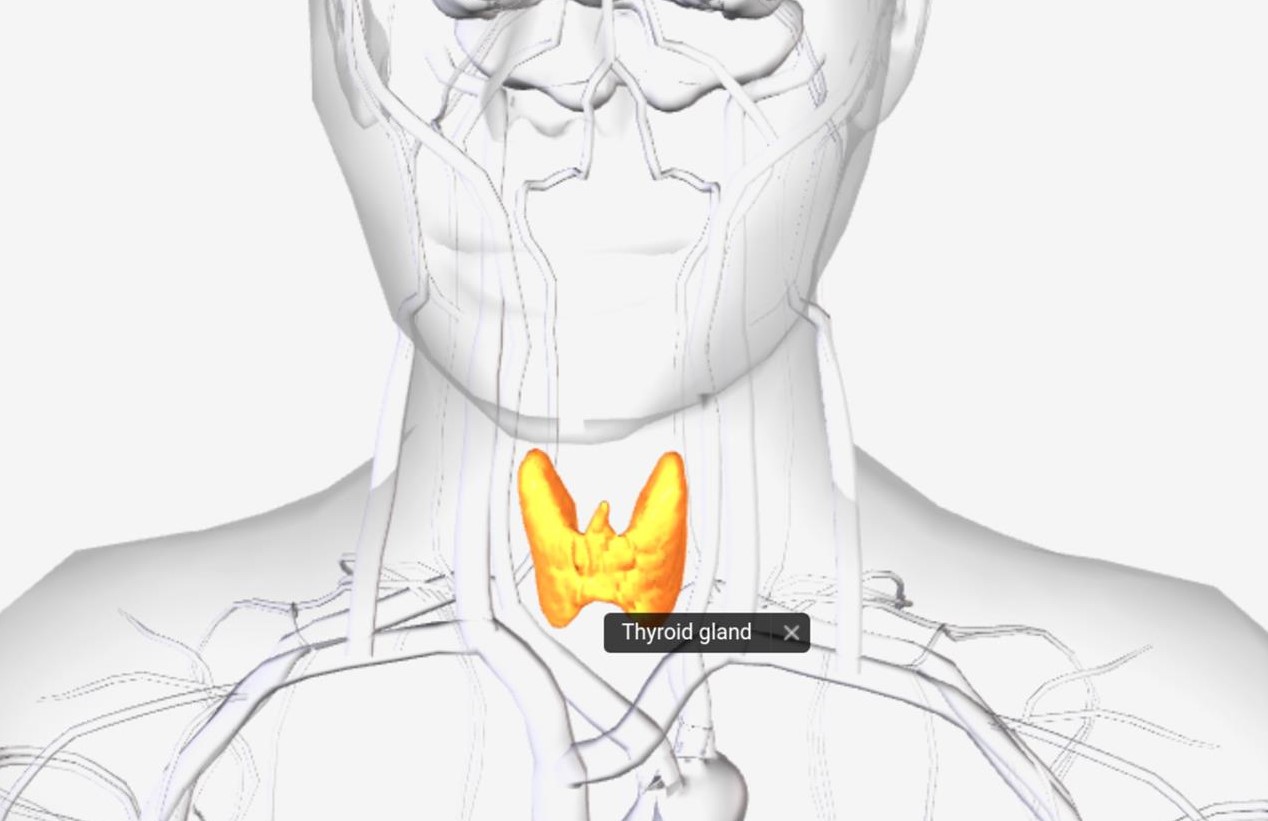
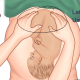
The thyroid gland is a butterfly-shaped structure located in front of the neck and inferior to the larynx, Adam’s apple. It consists of right and left lateral lobes, on either side of the trachea, connected by a narrow isthmus.
The thyroid weighs 25 grams and about 5 cm long, 3 cm wide and 2 cm thick, there are three primary features of the thyroid—follicles, follicular cells, and parafollicular cells, spherical sacs called thyroid follicles.
The wall of each follicle consists of follicular cells, which extend to the lumen of the follicle. A basement membrane surrounds each follicle.
The follicular cells produce two hormones- Tetraiodothyronine (T4), It contains four atoms of iodine, and Triiodothyronine (T3), which contains three atoms of iodine. Parafollicular cells or C cells lies between follicles. They produce the hormone calcitonin, which helps to regulate calcium balance.
Hormone Production-
Synthesis and secretion of T3 and T4 occurs as –
1) Iodide trapping-Thyroid follicular cells trap iodide ions (I–) from the blood into the cytosol.
2) Synthesis of Thyroglobulin- Follicular cells is synthesizing thyroglobulin(TGB), a glycoprotein that is produced in the rough endoplasmic reticulum, modified in the Golgi complex, and packaged into secretory vesicles. Then vesicles then undergo exocytosis, which releases TGB into the lumen of the follicle.
3) Oxidation of iodide– Negatively charged iodide ions cannot bind to tyrosine until they undergo oxidation (removal of electrons) to iodine. As the iodide ions are being oxidized, they pass into the lumen of the follicle.
4) Iodination of tyrosine– As iodine molecules (I2) form, they react with tyrosine. Binding of one iodine atom to tyrosine forms monoiodotyrosine (T1) & other iodination produces diiodotyrosine (T2). The TGB with attached iodine atoms accumulates in the lumen of the thyroid follicle, is termed colloid.
5) Coupling of T1 and T2– Two T2 molecules join to form T4, or one T1 and one T2 join to form T3.
6) Pinocytosis and digestion of colloid– Colloid then enter follicular cells by pinocytosis and merge with lysosomes. Lysosomal enzymes break down TGB & then T3 and T4 releases.
7) Secretion of thyroid hormones– T3 and T4 are lipid soluble, they diffuse through the plasma membrane into interstitial fluid and then into the blood.
8) Transport in the blood–both the T3 and the T4 combine with transport proteins in the blood.
Functions-
- Thyroid hormones increase basal metabolic rate (BMR), the rate of oxygen consumption, or the minimal rate of energy expenditure at rest. Use of cellular oxygen to produce ATP, so it increases, cellular metabolism of carbohydrates, lipids, and proteins increases.
- It helps in the maintenance of body temperature as it stimulates the synthesis of sodium-potassium pumps, which uses large amounts of ATP to eject sodium ions from the cytosol into the extracellular fluid and potassium ions from the extracellular fluid into the cytosol. So more heat is released, and body temperature rises.
- It stimulates protein synthesis, increases lipolysis and cholesterol excretion, thus reducing blood cholesterol levels.
- It increases sensitivity to catecholamines (norepinephrine and epinephrine which causes increased heart rate, increased blood pressure, increase blood glucose level.
- Synergic effect with human growth hormone and insulin, it increases body growth.
Control–
Low blood levels of T3 and T4 stimulates the hypothalamus to secrete TRH
⇓
TRH enters the hypophyseal portal veins and then to the anterior pituitary, where it stimulates thyrotrophs to secrete TSH
⇓
TSH stimulates hormone synthesis and secretion from follicular cells, then thyroid follicular cells release T3 and T4 into the blood
⇓
An elevated level of T3 and T4 inhibits the release of TRH and TSH secretion by negative feedback
Calcitonin–
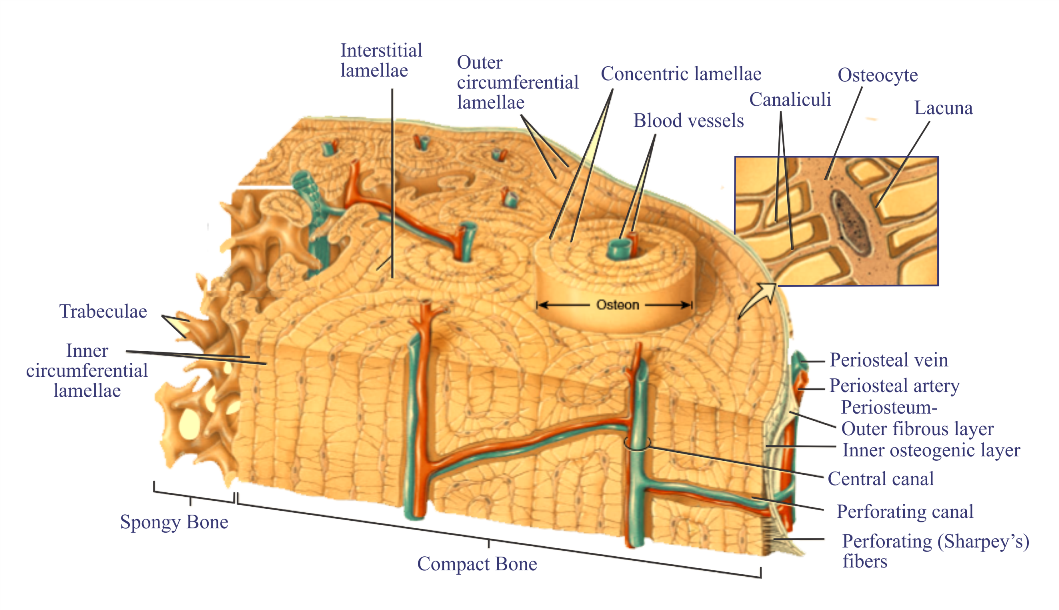
Another hormone release from parafollicular cells of the thyroid Gland is Calcitonin. It decreases the level of calcium in the blood by inhibiting the action of osteoclasts (a bone cell which absorbs bone tissue during growth and healing and which break down bone extracellular matrix).
Control–
When its blood level is high, calcitonin lowers the amount of blood calcium and phosphates by inhibiting bone resorption by osteoclasts.